Evaluating a Bispecific Monoclonal Antibody to Prevent Ventilator-Associated Pneumonia in Adult ICU Patients
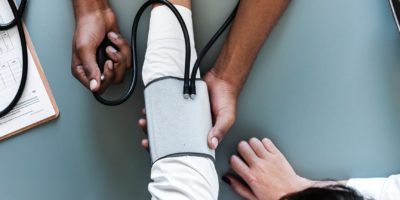
In November COMBACTE-MAGNET’s trial EVADE published a paper in the Critical Care Journal on the safety and efficacy of an investigational bispecific monoclonal antibody against two Pseudomonas aeruginosa proteins, for the prevention of ventilator-associated pneumonia in adult Intensive Care Unit (ICU)-patients.
The investigational drug is a first-in-class bivalent, bispecific human immunoglobulin G1 kappa monoclonal antibody that selectively binds to the P. aeruginosa PcrV protein and Psl exopolysaccharide involved in host cell cytotoxicity and P. aeruginosa colonisation and tissue adherence.
EVADE was a phase 2, single-dose, proof-of-concept study of the monoclonal antibody for the pre-emptive treatment of P. aeruginosa nosocomial pneumonia in mechanically ventilated patients with P. aeruginosa lower respiratory tract colonisation in the ICU, confirmed by a polymerase chain reaction (PCR)-based test on tracheal aspirates. The study did not meet the primary endpoint of reducing nosocomial P. aeruginosa pneumonia incidence in P. aeruginosa-colonised mechanically ventilated subjects.
Study design
“Our study involved several innovative methods. A pre-emptive trial design was employed to enrich the subject population for those at greatest risk of P. aeruginosa pneumonia. Respiratory tract colonisation was assessed by rapid polymerase chain reaction test on tracheal samples collected within 36 hours prior to randomisation. Study endpoints were developed in line with the pre-emptive design and in accordance with US Food and Drug Administration and the European Medicines Agency. An interim pharmacokinetic analysis was performed to evaluate the pharmacokinetic profile of the monoclonal antibody in mechanically ventilated critically ill patients”.
Antibodies as Prevention Strategy for Multi-drug Resistant Bacteria
Moreover, monoclonal antibodies represent a potential alternative to systemic antibiotics for the pre-emption of infections as they do not influence susceptibility to antibiotics.“There are currently no antibodies approved for the prevention of multi-drug resistant bacterial infections in the Intensive Care Unit” says one of the paper’s lead authors Prof. Jean Chastre, Groupe Hospitalier Pitié-Salpêtrière.

“Despite promising results in vitro and in animal models, we previously identified only one trial assessing the impact of a preventive strategy using a monoclonal antibody, and it did not show significant reduction of P. aeruginosa pneumonia. This illustrates the more general lack of strategies (preventive and/or curative) available to fight antimicrobial resistance”.
Further investigation is warranted into how monoclonal antibodies may benefit certain patient populations or be of use as an adjunctive therapy, overall reducing the need for antibiotics.
A Result of Collaboration between Academia and Pharma
Designing clinical trials to assess the safety and efficacy of anti-virulence agents is challenging from several standpoints and can be made more efficient by combining the forces and expertise of academia and pharma. The Innovative Medicines Initiative–funded COMBACTE consortium was able to foster such an academic-industry partnership between GHPS/CHU Limoges and AstraZeneca. This allowed to design a very relevant trial in accordance with the actual clinical scenario of pneumonia in ICU patients requiring mechanical ventilation at high risk of developing pneumonia caused by P. aeruginosa, and to deploy appropriate strategies to counteract as much as possible the difficulties in recruitment of appropriate subjects that are inherent in such a trial. Other advantages of this collaboration were access to and proper use of rapid diagnostic platforms at clinical sites, specimen collection and analysis, statistical considerations for determining population size, and identification of the most important and critical primary clinical end points, according to guidance from the U.S. Food and Drug Administration and the European Medicines Agency.
Related updates

Dr. Nithya Babu Rajendran Reflects On COMBACTE-MAGNET
Looking Back On COMBACTE-MAGNET